
Top 12 Agentic AI Healthcare Startups and Companies Transforming Enterprise Healthcare in 2026

The healthcare industry is placing enormous bets on agentic AI — and most of those bets are not paying off yet.
Sixty-one percent of healthcare leaders say they are already building and implementing agentic AI initiatives. Eighty-five percent plan to increase their investment over the next two to three years. AI agent startups raised $3.8 billion in 2024 alone, nearly triple the amount from the year before. Every major health system, payer, and life sciences company is either deploying autonomous agents or actively evaluating them.
But the production numbers expose a very different reality. Only 14% of enterprises have production-ready agentic AI systems. Gartner predicts that more than 40% of agentic AI projects will be cancelled by the end of 2027. The gap between experimentation and production is not shrinking — it is widening.
The problem is not a lack of startups. The healthcare AI market in 2026 is crowded with companies building agents for scheduling, imaging, documentation, revenue cycle, and patient communication. Many of them are excellent at what they do.
But analyst consensus across Deloitte, McKinsey, and Gartner points to a consistent root cause behind most failed deployments: healthcare AI agents are making decisions on incomplete context. They see the structured data — EHR records, billing codes, claims databases — but they are blind to the other 80% of enterprise healthcare data. The clinical notes. The contract PDFs. The policy documents. The faxed referrals. The physician emails. The compliance memos that change reimbursement rules overnight.
This is what separates the agentic AI healthcare startups that reach production from the ones that stall in pilot purgatory. Not the quality of their models. Not the size of their funding rounds. Whether their agents can see the full picture before making a decision.
This guide evaluates the 12 most significant agentic AI healthcare startups and companies in 2026 — not by buzz or funding alone, but by production readiness, governance, context completeness, and real clinical deployment outcomes. If you are a healthcare leader evaluating platforms, this is the list that tells you who is actually delivering and why.
How We Evaluated These Agentic AI Healthcare Companies

Most healthcare AI listicles rank companies by how much money they have raised or how many press releases they have published. That is a poor proxy for what actually matters when you are deploying autonomous agents in a healthcare environment where incorrect decisions affect patient care, regulatory compliance, and financial performance.
We evaluated every company on this list against five pillars that determine whether an agentic AI platform can survive the transition from demo to production in healthcare:
1. Context Completeness. Can the platform handle structured data (EHR, claims, billing) AND unstructured data (clinical notes, PDF contracts, faxed referrals, policy documents, physician emails)? Most AI tools see only 10–20% of enterprise healthcare data — the structured part sitting in databases. The other 80% is where the real clinical and operational truth lives. We call this The 80/20 Data Problem, and it is the single most common reason healthcare AI agents fail in production.
2. Governance and Auditability. Are agent decisions deterministic — meaning rule-based, reproducible, and traceable to a specific policy or compliance requirement? Or are they probabilistic — meaning the LLM generates an output that might vary each time with no audit trail? Healthcare demands the former. Every claim approval, staffing decision, prior authorisation, and compliance determination must be explainable and defensible.
3. Autonomous Execution. Does the agent reason AND act? Or does it recommend actions and leave humans as the bottleneck? A copilot that recommends still requires the same headcount to execute. True agentic AI closes the loop between insight and action within governed parameters.
4. Production Deployments. Is this platform running on real patient data in live healthcare environments today? Or is the evidence limited to pilots, demos, controlled environments, or press releases about future capabilities?
5. Compliance and Security. HIPAA compliance, SOC2 Type II certification, ISO 27001 alignment, data residency controls, encryption standards, and critically — whether the vendor trains its models on customer data. In healthcare, security is not a feature. It is a prerequisite.
Every company on this list has genuine strengths. Not all of them meet every criterion. The evaluation framework is designed to help you understand what each platform does well and where its limitations lie — so you can match the right solution to your specific healthcare use case.
The 12 Best Agentic AI Healthcare Startups and Companies in 2026
1. Hippocratic AI — Safest Voice Agents for Patient Communication
Hippocratic AI has built one of the most recognised brands in healthcare agentic AI by doing something most companies in the space avoid: drawing a hard line around what their agents will and will not do.
Their AI agents do not diagnose. They do not prescribe. They operate exclusively in areas the company believes generative AI can safely handle — and that constraint is exactly what has earned them the trust of major health systems. With over 150 million reported clinical interactions, a $141 million Series B that earned them unicorn status, and deployments across large hospital networks, Hippocratic AI is the most prominent agentic AI healthcare startup focused on patient communication.
Their agents handle outbound patient calls for chronic care management, medication adherence, post-discharge follow-up, care gap closure, wellness visit scheduling, and screening reminders. The technology uses voice agents that can recognise subtle cues about symptoms and escalate to human nurses when needed. They run seasonal vaccination campaigns, conduct RPM adherence check-ins, and handle inbound calls for basic patient questions — all with empathetic, first-ring support.
The governance model is built around clinical guardrails rather than enterprise governance. Agents stay within strictly defined clinical scopes and escalate anything outside those boundaries to human clinicians.
Best for: Health systems and provider organisations that need to scale patient outreach, chronic care management, and care gap closure without adding headcount to already-strained nursing teams.
Where it fits and where it doesn't: Hippocratic AI is the clear leader in patient-facing voice agents. However, the platform is not designed for operational analytics, revenue cycle automation, multi-system enterprise orchestration, or fusing unstructured enterprise data like contracts, compliance policies, and cross-departmental communications. If your primary challenge is patient communication at scale, Hippocratic AI is the frontrunner. If your challenge is enterprise-wide operational decision-making across fragmented data sources, you will need a different architecture.
2. Assistents.ai (Ampcome) — Context-Complete Governed Agents for Enterprise Healthcare Operations
While most agentic AI healthcare startups focus on a single workflow — scheduling, imaging, documentation, or billing — Assistents.ai is built around a fundamentally different premise: agents should never make a decision without seeing the full picture first.
This is the only platform on this list specifically engineered to solve The 80/20 Data Problem in healthcare. Most AI tools connect to structured data sources — EHR systems, claims databases, billing platforms — and treat that as sufficient context. But structured data represents only 10–20% of what healthcare organisations actually know. The other 80% lives in clinical notes, PDF contracts with payer-specific coverage terms, faxed referrals with critical patient history, physician emails clarifying treatment necessity, policy documents that change reimbursement rules, and compliance memos scattered across SharePoint, Slack, and email.
An agent processing a claim that cannot see the contract exception for that procedure, or approving a staffing match without verifying facility-specific compliance requirements, or routing a patient workflow without understanding the policy update that changed the process last week — that agent is operating on a fraction of what it needs.
Assistents.ai addresses this through a three-tier architecture called the Autonomy Stack:
Tier 1: Unified Context Engine. This engine fuses structured data (EHR, claims, billing, HR systems) with unstructured data (clinical notes, PDF contracts, faxed referrals, email threads, policy documents, compliance memos) and external data (regulatory updates, formulary changes, payer policy revisions) into a single semantic layer. Agents query this layer before making any decision — meaning they see the complete picture, not just the 20% that sits in databases.
Tier 2: Semantic Governor. Every agent decision passes through a deterministic governance layer. This is not probabilistic LLM output — it is rule-based, auditable, and policy-cited. The governor encodes approval hierarchies, compliance thresholds, and if-then decision trees defined by the healthcare organisation. Every action is traceable to a specific rule. Every decision is explainable and defensible. Human-in-the-loop controls are configurable: routine decisions below defined thresholds run fully autonomously, while high-value or high-risk decisions escalate to human review.
Tier 3: Active Orchestrator. The orchestration engine executes multi-step workflows across enterprise systems — EHR, billing, HR, compliance, scheduling, and communication platforms — in a single governed workflow. It does not replace existing systems. It sits on top of them, coordinating agents that navigate across platforms to complete end-to-end processes.
Production healthcare deployments (organisations anonymised):
A physician-led clinical enterprise running hospitalist programs across multiple care facilities deployed governed agents for revenue management and operational analytics. The context engine unified billing data, HR records, scheduling platforms, clinical notes, and care-program documentation into a single layer. Result: improved visibility into revenue leakage, faster operational decision-making, and cross-facility performance tracking that was previously impossible when data lived in disconnected systems.
A healthcare staffing platform connecting nursing professionals with facilities automated the full matching workflow — from intake to credential verification to shift assignment to compliance documentation. Agents could see credential databases, facility-specific compliance requirements, scheduling feeds, and historical performance data simultaneously. Result: faster fill cycles, lower scheduling friction, compliance verification built into every match rather than checked after the fact.
A private diagnostics provider processing thousands of bookings, tests, and results weekly deployed agents that orchestrated the end-to-end patient journey — booking through result delivery — with automated monitoring at every handoff point. Result: reduced manual overhead, fewer missed handoffs, faster patient communications, and proactive bottleneck identification.
A geriatric care services provider across assisted living and long-term care settings unified programme operations, staffing, service delivery, and revenue data into a single analytics layer. Governed agents surfaced revenue cycle exceptions in days rather than weeks and correlated staffing patterns with care outcomes across facilities.
Compliance: SOC2 Type II, ISO 27001 aligned, HIPAA compliant, GDPR compliant, AES-256 and TLS 1.3 encryption, no training on customer data. Deployable cloud, private, on-premise, or hybrid.
Deployment speed: Pilot to production in 30 days.
Best for: Healthcare organisations that need agents acting on complete enterprise context — not just EHR data — with deterministic governance and full audit trails. Particularly strong for multi-facility clinical operations, healthcare staffing, diagnostic workflow orchestration, and organisations where unstructured data is critical to decision quality.
Where it fits and where it doesn't: Assistents.ai is the strongest option on this list for enterprise-wide healthcare operations where agents need to fuse data across multiple systems and data types. It is not a point solution for a single workflow like radiology triage or physician documentation — it is infrastructure for organisations where the context problem is the bottleneck preventing agents from reaching production.
3. Assort Health — Omnichannel Patient Engagement AI
Assort Health has carved out a strong position in one of healthcare's most persistent operational pain points: the front desk.
Their AI agents handle inbound and outbound patient calls across scheduling, prescription refills, billing inquiries, and general patient FAQs. What makes Assort Health stand out among agentic AI healthcare startups is the depth of customisation — their system is tailored by organisation, specialty, provider, and even region, with over 1.1 million workflows developed from tens of millions of patient interactions.
The reported results are significant. Organisations using Assort Health have seen hold times drop from 11 minutes to under one minute, call abandonment rates reduced by 57%, and labour capacity increased by 48%. The platform is deployed across orthopedics, cardiology, dermatology, primary care, pediatrics, ophthalmology, urology, and more — handling scheduling across 100+ providers and six specialties at some organisations.
The AI handles call triage, FAQ resolution, appointment scheduling with provider-specific logic, prescription refill requests, billing questions, fax automation, and waitlist management. It also supports campaign-based outreach via text, email, and voice for waitlist management, appointment reminders, and recall campaigns.
Best for: Multi-specialty practices and health systems drowning in call volume that need immediate front-desk relief with specialty-specific customisation.
Where it fits and where it doesn't: Assort Health excels at patient access and front-office automation. It does not address back-office operational analytics, claims processing, multi-system enterprise orchestration, or the kind of cross-departmental data fusion required for complex operational decision-making.
4. Notable Health — Revenue Cycle and Care Operations AI Agents
Notable Health positions itself as a full-platform approach across three interconnected domains: patient access, revenue cycle management, and care operations. Their AI agents automate prior authorisations, copay estimation and collection, intake and registration, referral management, care gap outreach, and pre-procedure instructions.
The platform's strength lies in connecting these workflows rather than treating them as isolated automation targets. An agent that handles intake can feed information directly into the revenue cycle workflow, which connects to care operations for follow-up. This reduces the handoffs and data re-entry that plague most healthcare administrative processes.
Notable specifically targets the financial side of healthcare operations — denial prevention, appeal letter generation, patient estimates with real-time eligibility verification, and claims management. The focus on measurable financial ROI (reduced denial rates, faster billing cycles, lower administrative burden) makes their value proposition straightforward for CFOs and revenue cycle leaders.
Best for: Healthcare organisations where revenue cycle inefficiency is the primary pain point and agents need to connect access, billing, and care operations.
Where it fits and where it doesn't: Strong on administrative and financial workflows. Less focused on clinical operations analytics, physician-facing tools, or fusing unstructured clinical data for enterprise-wide decision-making across non-financial domains.
5. VoiceCare AI — Agentic Voice Agents for Provider-Payer Communication
VoiceCare AI addresses what might be the single most tedious workflow in all of healthcare: sitting on hold with insurance companies.
Their AI agent, Joy, makes outbound calls to payers for benefit verifications, prior authorisations, claims follow-ups, and prescription support. The agent can navigate interactive voice response (IVR) systems, handle transfers between multiple human representatives, and stay on calls for up to two and a half hours — which, in healthcare back-office operations, is not unusual.
The startup kicked off a pilot with Mayo Clinic to automate patient pre-authorisation and benefit confirmations within neurology and pediatrics departments. With $3.8 million in funding and a HIPAA-compliant, SOC2 Type II attested platform, VoiceCare AI is early-stage but tackling a problem that consumes staggering amounts of healthcare staff time. Studies show clinicians spend nearly 28 hours per week on administrative tasks, while medical office and claims staff spend 34 and 36 hours respectively.
Best for: Provider organisations with large revenue cycle teams spending hours daily on phone calls with payers for verifications, authorisations, and claims follow-up.
Where it fits and where it doesn't: Narrow but deep. VoiceCare AI is purpose-built for phone-based payer communication. It does not handle patient-facing workflows, clinical documentation, operational analytics, or multi-system enterprise orchestration. Think of it as a specialist tool for one of healthcare's most painful specific workflows.

6. Qure.ai — AI Agents for Diagnostic Imaging
Qure.ai is one of the most established agentic AI healthcare companies in the diagnostic imaging space. Their FDA-cleared AI agents analyse X-rays, CT scans, and MRIs in real time — detecting abnormalities, triaging critical cases, and reducing the workload on radiologists who are increasingly stretched thin.
The platform's core strength is clinical-grade accuracy in time-sensitive imaging scenarios. For critical cases like strokes, pulmonary embolisms, and cervical spine fractures, the agent identifies the finding and flags it for immediate radiologist review — cutting the turnaround time for cases where minutes matter. Beyond emergency triage, Qure.ai's agents support tuberculosis screening, chest X-ray analysis, and head CT interpretation at population scale.
With deployments across multiple countries and FDA clearance for its core products, Qure.ai has moved well beyond the pilot stage. Their global footprint makes them one of the more proven agentic AI companies in healthcare, particularly in markets where radiologist shortages make AI-assisted triage essential rather than optional.
Best for: Hospitals and imaging centres with high radiology volumes that need AI-assisted triage to prioritise critical cases and reduce turnaround times.
Where it fits and where it doesn't: Qure.ai is an imaging specialist. It does not address healthcare operations, workflow automation, revenue cycle management, patient communication, or enterprise data challenges. If your primary bottleneck is radiology, it is a proven solution. If your challenges span multiple departments and data types, you need a broader platform.
7. Innovaccer — Health Data Platform with Agentic Capabilities
Innovaccer's approach to healthcare agentic AI starts from a data unification premise rather than a workflow automation premise. Their Health Data Platform aggregates and normalises patient data across EHR systems, claims databases, and other clinical sources — creating a unified patient view that then supports AI agent capabilities for care management and population health.
The agentic layer is applied to specific high-value workflows, particularly referral management. Innovaccer's agents automate the end-to-end referral process — matching patients with appropriate specialists, reducing network leakage, and ensuring follow-through. In a value-based care environment where providers are financially responsible for patient outcomes beyond the initial visit, automated referral management directly impacts the bottom line.
Additional use cases include care gap closure, population health analytics, and patient engagement — all built on top of the unified data layer. The data-first approach means Innovaccer often appeals to organisations that have an existing data fragmentation problem and want to solve it as a prerequisite to deploying AI agents.
Best for: Healthcare organisations that need to unify fragmented patient data across systems as a foundation for AI-driven care management and population health.
Where it fits and where it doesn't: Innovaccer is primarily a data platform with agent capabilities layered on top. The autonomous execution and governance capabilities are less mature than purpose-built agentic platforms. It is strongest as a data unification and care coordination play — less suited for organisations that need agents executing complex, multi-step workflows across non-clinical enterprise systems.
8. Suki AI — AI Agent for Physician Documentation
Suki AI focuses on the clinician's daily experience — specifically, the documentation burden that consumes hours of physician time and contributes directly to burnout.
Their AI agent is voice-activated and physician-facing. During patient encounters, physicians can call out to Suki to access medications, vital signs, allergies, surgical histories, and other clinical information instantly. The agent can also complete tasks autonomously — ordering labs, setting up follow-up visits, sending appointment reminders — based on voice commands during or after the patient interaction.
At a list price of $399 per user per month, Suki positions itself as a direct productivity tool for individual clinicians rather than an enterprise infrastructure play. The value proposition is straightforward: reduce documentation time, give physicians back hours each day, and reduce the administrative burden that drives clinician turnover.
The approach is deliberately focused. Suki does not try to orchestrate enterprise workflows, manage revenue cycles, or unify data across departments. It solves one problem — physician documentation and in-workflow task completion — and aims to solve it exceptionally well.
Best for: Physician groups and health systems where clinician burnout driven by documentation burden is the most urgent problem to solve.
Where it fits and where it doesn't: Suki is a physician-facing tool. It does not address operational analytics, claims processing, staffing, compliance automation, or enterprise-wide data challenges. If your priority is making individual physicians more productive, Suki is a strong fit. If your challenges are organisational and operational, you need a platform with broader scope.
9. Thoughtful AI — Revenue Cycle Automation
Thoughtful AI takes the full revenue cycle — one of the most complex, error-prone, and costly workflows in healthcare — and applies end-to-end agentic automation to it.
Their platform handles eligibility checks, benefit verification, claims submission, denial management, and appeals processing. What elevates Thoughtful AI above traditional RCM automation is the intelligence layer: real-time reporting on denial trends, coding accuracy monitoring, and workflow efficiency analytics that help organisations identify and fix systemic revenue cycle issues rather than just processing individual claims faster.
In an industry where claim denials cost the average hospital millions per year and the denial rate continues to climb, agentic AI that can not only process claims but also identify patterns, predict denials before they happen, and automatically generate appeals represents a meaningful step forward from scripted RPA.
Best for: Healthcare organisations with large revenue cycle operations where denial rates, coding errors, and claims processing speed are critical financial metrics.
Where it fits and where it doesn't: Revenue cycle is the exclusive focus. Thoughtful AI does not address clinical operations, patient communication, physician documentation, or multi-department enterprise workflows. If RCM is your biggest operational challenge, this is a dedicated solution. If you need agents operating across clinical, operational, and financial domains simultaneously, you need a broader platform.
10. Hyro — Conversational AI for Healthcare Contact Centres
Hyro builds adaptive conversational AI agents that operate across voice, chat, and SMS — specifically designed for healthcare contact centres managing high patient call volumes.
Their agents handle appointment scheduling, patient FAQ resolution, eligibility screening, and general inquiry routing. Hyro has positioned itself around the compliance implications of recent healthcare regulations, arguing that proactive patient engagement is becoming a regulatory requirement rather than just a competitive advantage.
The adaptive conversation model is a differentiator — Hyro's agents are designed to work across multiple healthcare specialties and organisations without extensive custom training for each deployment. This makes the platform appealing for health systems that need to deploy quickly across multiple departments or facilities.
Best for: Health systems with overwhelmed contact centres that need AI to manage high call volumes across voice, chat, and SMS channels.
Where it fits and where it doesn't: Hyro is a communication and contact centre solution. It does not handle clinical analytics, enterprise data fusion, revenue cycle automation, or multi-step operational workflows that span beyond the patient communication layer.
11. Aidoc — AI Triage for Radiology
Aidoc provides always-on AI triage for medical imaging, with a specific focus on identifying time-critical findings that require immediate radiologist attention.
The platform analyses radiology scans in real time, flagging critical conditions — strokes, pulmonary embolisms, cervical spine fractures, intracranial haemorrhages — and reprioritising the radiologist's worklist accordingly. In a specialty where reading order can directly impact patient outcomes, this reprioritisation is the agent's most valuable function.
Aidoc has FDA clearance across multiple clinical indications and is deployed in hospitals globally. The technology is mature and clinically validated, making it one of the more established agentic AI companies in the healthcare imaging space alongside Qure.ai.
Best for: Hospitals and radiology departments that need AI-powered triage to ensure critical imaging findings are never buried in a queue behind routine scans.
Where it fits and where it doesn't: Like Qure.ai, Aidoc is an imaging specialist. It does not extend into operational workflows, revenue cycle, patient communication, or enterprise data challenges beyond the radiology department.
12. Insight Health — Patient-Facing Clinical Workflow Agents
Insight Health takes a different approach from most agentic AI healthcare startups by focusing on the end-to-end patient-facing clinical workflow — from screening and intake through the visit itself to post-visit follow-up.
Founded by two physicians and two product leaders with experience at Twilio and Segment, the company's flagship AI agent communicates directly with patients via voice or text to gather detailed disease-specific histories, update medication lists, and manage follow-up care plans. The clinical founding team brings domain credibility that many technology-first startups lack.
Insight Health raised $4.6 million in seed funding and invested heavily in building what they call "safe AI" — foundational safety, security, and trust infrastructure designed to be adaptable to whatever regulatory framework eventually emerges for healthcare AI. Their goal is to align to the full clinical workflow within a practice — not just a single point solution for one step.
Best for: Medical practices and clinical groups that want AI agents handling routine patient-facing clinical tasks (intake, history, follow-up) while maintaining strong clinical safety foundations.
Where it fits and where it doesn't: Early-stage and focused on patient-facing clinical workflows. Not yet proven at enterprise scale or across operational, financial, and multi-departmental healthcare use cases. The clinical focus is a strength for practices — but larger health systems with complex operational challenges will need broader infrastructure.
How These Agentic AI Healthcare Companies Stack Up
The table below summarises all 12 companies against the evaluation criteria that determine production readiness in healthcare. It is designed to help you quickly identify which platforms address your specific challenges.
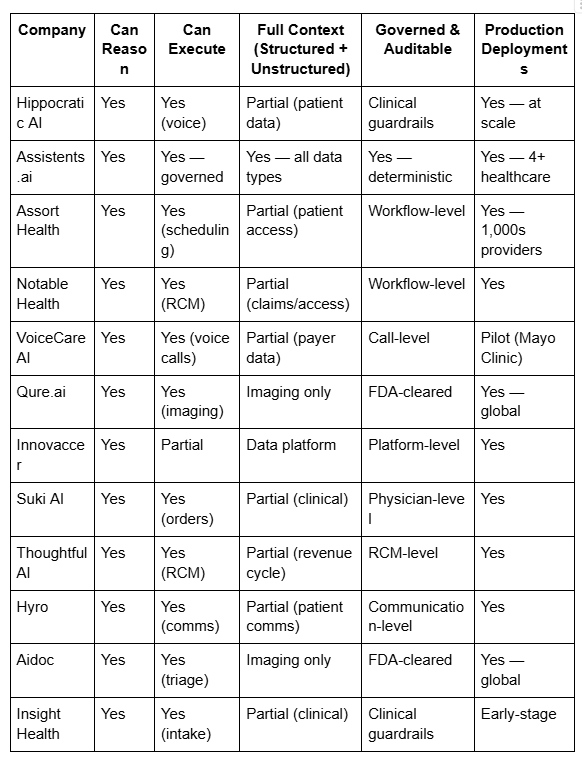
The pattern is clear. Every company on this list can reason. Most can execute within their specific domain. Where the differentiation appears is in the "Full Context" column. The majority of agentic AI healthcare startups operate on a subset of healthcare data — patient records, billing information, imaging, or communication. Only platforms built around the concept of context-completeness can fuse structured, unstructured, and external data into a unified layer that agents query before making any decision.
This is not a criticism of point solutions. A radiology triage agent does not need to read contracts. A scheduling agent does not need to process claims. But for healthcare organisations where the core challenge is enterprise-wide operational decision-making — where agents need to see clinical data, financial data, compliance data, and unstructured documents simultaneously — the context column is what separates production from pilot.
AI Healthcare Companies in India: The Growing Governed Agent Ecosystem
India's healthcare market is one of the most demanding proving grounds for agentic AI in the world — and the companies that succeed here are building capabilities that translate globally.
The scale alone is staggering. India's doctor-to-patient ratio sits at approximately 1:1263. The Ayushman Bharat programme provides health coverage to over 500 million citizens. Hospitals in India routinely process patient volumes that would overwhelm most healthcare systems globally. The administrative burden is massive, the regulatory environment is evolving rapidly, and the workforce shortage is acute across every clinical and operational function.
For agentic AI healthcare companies, India is not just a market — it is a stress test. Healthcare data in India is more fragmented than in most Western markets. Paper records coexist with digital systems. Multiple languages are in active use within the same patient journey. Government and private sector systems rarely share data standards. Faxed documents, handwritten prescriptions, and phone-based referrals remain common across many care settings.
An agentic AI platform that can only process structured EHR data is fundamentally inadequate in an Indian healthcare environment where a significant portion of clinical truth lives on paper, in regional-language notes, or in verbal communications between providers.
Several production deployments in India demonstrate what context-complete governed agents can achieve at this scale. One deployment covers smart city health and utility infrastructure spanning 25+ city operation centres and over 2 million connected assets, serving more than 150 million urban lives with AI agents replacing reactive dashboard monitoring with proactive alerting. Multiple clinical operations deployments across India have automated workflow support, revenue cycle monitoring, and operational analytics — handling the multi-lingual, multi-system complexity that defines Indian healthcare. Enterprise healthcare analytics deployments have unified cross-entity operations spanning multiple geographies, standardising KPIs and surfacing operational insights that were invisible when data lived in disconnected systems.
The companies that prove context-completeness at Indian healthcare scale — with its data fragmentation, linguistic diversity, and operational complexity — carry a significant competitive advantage for global deployments. If the platform works in India, it can work anywhere.
The Blind Agent Problem — What Every Healthcare Buyer Must Understand Before Choosing a Platform
Before selecting any agentic AI healthcare startup from this list — or any other — every healthcare leader needs to understand the root cause behind most failed healthcare AI deployments. It is not a model problem. It is a context problem.
We call it The Blind Agent Problem, and it works like this.
AI agents are amplifiers. They do not create order or chaos — they multiply whatever already exists. When they operate on clean, complete data with clear governance rules, they multiply efficiency at speeds no human team can match. When they operate on fragmented data with partial context, they multiply chaos. And they do it faster than anyone can intervene.
Only 10–20% of healthcare enterprise data lives in the structured systems that most AI tools can access — the EHR tables, claims databases, and billing platforms. The other 80% is unstructured: clinical notes dictated by physicians, PDF contracts with payer-specific coverage exceptions, faxed referrals containing critical patient history, email threads between billing departments and payer representatives clarifying rate changes, policy update memos that alter authorisation requirements, compliance documents scattered across SharePoint and shared drives.
This is The 80/20 Data Problem, and it is the defining challenge for healthcare agentic AI in 2026.

Consider what happens in practice. An AI agent is deployed to automate insurance claim processing. It has access to billing codes, patient records, treatment dates, provider information, and payer details. It processes efficiently and confidently. But it cannot see the contract PDF that specifies a coverage exception for that procedure. It cannot read the physician's email explaining why a non-standard treatment was medically necessary. It does not know about the policy update that changed pre-authorisation requirements last month.
The agent approves, denies, or routes the claim based on 20% of the available context. Many of those decisions look correct on the surface. But the contract exception is missed. The negotiated rate is ignored. The clinical justification is never considered. The result: denied claims that should have been approved. Approved claims at incorrect rates. Compliance violations that trigger audits. Revenue leakage that compounds across thousands of claims per month.
This is not a hypothetical scenario. Across industries, agents operating on incomplete context have generated real financial damage — including one documented case where an AI agent approved over ₹12 crore in early vendor payments, executing flawlessly based on the ERP data and invoices it could see while completely blind to contract terms, negotiated discounts, and cash flow warnings that lived in PDFs, emails, and internal messages.
In healthcare, the stakes are higher. A claims agent acting on incomplete data does not just lose revenue — it delays patient care, triggers regulatory scrutiny, and erodes the trust between payers and providers that the entire system depends on.
Deloitte specifically identified data fragmentation as a key healthcare challenge in their 2026 analysis. Agents given too much scope without proper context become prone to errors that compound at enterprise speed. The organisations on this list that address the full-context problem — that build agents capable of seeing structured and unstructured data simultaneously — are the ones reaching production. The ones that do not are contributing to the 40% cancellation rate that Gartner predicts.
How to Choose the Right Agentic AI Healthcare Startup for Your Organisation
After evaluating the 12 companies on this list, narrow your choice by asking these seven questions. They separate production-grade healthcare AI platforms from tools that will stall between pilot and deployment.
1. Does the platform see ALL your data — structured AND unstructured? If the vendor says "we connect to your EHR," ask specifically about contract PDFs, clinical notes, faxed referrals, policy documents, and cross-departmental email threads. If those are invisible to the agent, it is operating on a fraction of what it needs.
2. Can agents execute decisions — or do they only recommend? A copilot that recommends actions still requires the same number of humans to execute them. True agentic AI closes the loop within governed parameters.
3. Is governance deterministic or probabilistic? Deterministic means rule-based, reproducible, and auditable every time. Probabilistic means the LLM generates an output that might vary with no audit trail. Healthcare compliance demands deterministic governance.
4. Does every decision come with a full audit trail and policy citation? Not just what was decided — but why it was decided, which rule authorised it, and which compliance requirement it satisfied. This is non-negotiable for HIPAA and regulatory audits.

5. Can you go from pilot to production in 30 days with real enterprise data? Any vendor can run a demo on sanitised data. Ask for a timeline to production with your actual data, your actual systems, and your actual compliance requirements.
6. Does the platform support configurable human-in-the-loop thresholds? Healthcare requires graduated autonomy. Routine decisions might be fully autonomous. High-value exceptions require human review. The thresholds should be defined by your organisation — not hardcoded by the vendor.
7. Show me production case studies in healthcare — not demos. Demos prove capability. Production case studies prove reliability. Ask for evidence of agents running in live healthcare environments on real data with measurable outcomes.
Any platform that cannot give you a clear, specific answer to each of these questions deserves deeper scrutiny before you commit budget and operational resources to a deployment.
See Your Healthcare Context Gap in 48 Hours
If your healthcare organisation is evaluating agentic AI — or stuck between pilot and production — start with the context problem.
Within 48 hours, receive a concrete pilot plan: workflow definition for your highest-value use case, ROI hypothesis based on your actual data landscape, success metrics tied to operational outcomes, and a clear timeline from assessment to production.
If the assessment does not surface real, new value — walk away. No POC purgatory. No six-month evaluations. The enterprises running governed agents in production today all started the same way: by seeing how much of their data their agents could not see.
The organisations reaching production with agentic AI in 2026 share one trait: they identified their context gap before they built their architecture. They did not discover mid-deployment that their agents were operating on 20% of available data.
If you are evaluating platforms or troubleshooting a stalled pilot, a structured context assessment is often the fastest way to identify why agents are underperforming — and what it would take to close the gap. Most healthcare leaders who complete one find the answer is simpler than they expected.
[Book Your 48-Hour Context Assessment →]
Frequently Asked Questions
What are the top agentic AI healthcare startups in 2026?
The top agentic AI healthcare startups in 2026 include Hippocratic AI for patient voice agents, Assistents.ai for context-complete governed enterprise agents, Assort Health for patient engagement, Notable Health for revenue cycle, VoiceCare AI for payer communication, Qure.ai for diagnostic imaging, and Suki AI for physician documentation — each addressing different segments of healthcare operations.
What is the difference between healthcare copilots and agentic AI?
Copilots recommend actions and require humans to execute. Agentic AI reasons, decides, and executes autonomously within governed parameters. Copilots typically access structured data only. Context-complete agentic AI fuses structured, unstructured, and external data — giving agents the full picture before they act.
Why do healthcare AI agent projects fail?
Healthcare AI projects fail primarily due to context gaps — agents making decisions on structured EHR and billing data while unable to see clinical notes, contract PDFs, policy documents, and cross-system communications. This is The 80/20 Data Problem, causing incorrect approvals, compliance violations, and stalled production deployments.
What is governed AI in healthcare?
Governed AI means every agent decision is deterministic, auditable, and policy-cited. Decisions are rule-based and reproducible rather than probabilistic LLM outputs. Every action is fully traceable, linked to specific compliance requirements, and includes configurable human-in-the-loop controls for high-risk actions.
What is The 80/20 Data Problem in healthcare AI?
Only 10–20% of healthcare data lives in structured systems like EHR and claims databases. The other 80% — clinical notes, contracts, policy documents, faxed referrals, physician emails — is unstructured and invisible to most AI agents, causing decisions based on incomplete information.
Which AI healthcare companies operate in India?
India's healthcare AI market includes companies deploying governed agents for clinical operations, smart city health infrastructure covering over 150 million urban lives, and healthcare staffing platforms. The most advanced handle India-specific challenges including multi-lingual data, paper-to-digital transitions, and massive patient volumes.
How do you evaluate an agentic AI healthcare startup?
Evaluate on five dimensions: data completeness (structured AND unstructured), governance (deterministic rules rather than probabilistic outputs), execution capability (acts, not just recommends), audit trail (every decision traceable to a policy), and deployment speed (pilot to production in 30 days or less).
Can agentic AI replace healthcare workers?
Agentic AI augments healthcare workers rather than replacing them. It automates administrative burden — claims, scheduling, compliance monitoring, revenue cycle management — so clinicians focus on patient care. The best platforms include graduated human-in-the-loop controls, handling routine decisions autonomously while escalating complex or high-risk cases to human professionals.

Transform Your Business With Agentic Automation
Agentic automation is the rising star posied to overtake RPA and bring about a new wave of intelligent automation. Explore the core concepts of agentic automation, how it works, real-life examples and strategies for a successful implementation in this ebook.
More insights
Discover the latest trends, best practices, and expert opinions that can reshape your perspective
Contact us












